

Nimble, mobile, informed and connected
Community-led responses
As part of the “Community-led responses” chapter, we highlight the work of communities around the world.
SCROLL DOWN
As seen recently during the COVID-19 pandemic, community-led organizations have mobilized when and where governments could not. Groups led by and for people living with HIV and key populations, including women and young people, leveraged in-depth HIV knowledge into broader pandemic expertise.
From Cote d’Ivoire to China, civil society groups distributed antiretroviral medicines (by post or hand-delivery) and self-testing kits, negotiated with government officials to ensure that medicines would be accessible and distributed food package and other essentials.
Many others from Botswana to Belgium also reported shifting their services online, as well as relying on telephone and email contact for personal counselling and monitoring of health status, with some even making home visits in urgent circumstances.
In Ukraine, for instance, many life-saving health services could not operate after the breakout of the war.

But grassroot providers such as the Alliance for Public Health found ways to keep going. Despite roads being mined and many bridges having been blown up, the Mobile HIV Case-Finding project used its 16 vans to deliver food, HIV treatment and other essentials across the country. It also helped people find shelter.
Iryna, the Coordinator of the mobile clinic team in the Chernihiv region, said the war had complicated its work immensely. Chernihiv borders the Russian Federation and Belarus in northern Ukraine.
“Many people were on the move, going from one place to another,” she said. “It was very difficult to work.”
But since mid-March, the Alliance for Public Health has restored many of its services. The nongovernmental organization works mainly with people who inject drugs and their partners.
“A substantial number of new HIV cases in Ukraine are registered among injecting drug users because of unsafe injecting practices,” explains the UNAIDS Country Director for Ukraine, Raman Hailevich.
He knows that reaching drug users was a challenge before the war, and it’s an even greater challenge now. The credit, he said, goes to civil society groups.
“Community-based organizations working with this type of hard-to-reach population provide the most essential outreach to these groups. Without them, the delivery of prevention programmes among people who use drugs would not be possible,” he said.
Because of the insecurity, the Alliance for Public Health saw a drop in testing for HIV and hepatitis C. Iryna, however, is proud because, she said, the teams delivered treatment to more than 1400 people in March and April through the mail and/or personal home delivery.

Since 2014, Venezuela has suffered the deepest economic depression and largest forced displacement with six million of its citizens fleeing the country. Political turmoil and international sanctions have meant that people have been struggling with food and basic essentials. The country’s health system has also collapsed. When Teresa (not her real name) arrived in Caracas she weighed 30 kilos. She had not been able to get HIV treatment due to massive stock shortages.
Led by the Venezuelan Network of Positive People (RVG+) and Acción Ciudadana Contra el Sida (ACCSI), along with more than 20 Venezuelan civil society organisations, they united to strengthen community outreach and monitoring of people living with HIV. Incorporating a system known as KoBo ToolBox—a free and open-source, solar-powered platform for collecting and managing data in challenging environments and humanitarian emergencies— they have real-time data regarding treatment, patient needs and other information.
Regina Lopez, UNAIDS Country Director in Venezuela, hails this collaborative effort as historic. “The project made it possible to recover and link many people who stopped receiving treatment in 2018 and those who returned to the country after several waves of migration,” she said.
This community outreach applies to basic services in stable countries too.
In a suburb of Nouakchott, Mauritania, a tent has gone up for an evening of counselling and HIV testing (see video). Staff of the nongovernmental organization SOS Pairs Educateurs field questions, and people wanting to know their HIV status queue for a rapid test.
To reach out to key populations, SOS PE, with the support of the United Nations and partners, recently opened a drop-in centre in front of the bus station in the capital city (they have eight other drop-in centres around town). A television blasts in the corner as peer educators mill about chatting with a truck driver. A pilot project distributing HIV self-test kits that people can use in the privacy of their own home has also been launched.

According to the UNAIDS Country Director for Mauritania, El Mustapha Attighie, community outreach like this is a way to support vulnerable groups.
“Stigma hinders our response to HIV and if human rights are not respected and people are left behind, this increases the risks of HIV,” he said. He added that UNAIDS’ mandate clearly states advocating for rights and treatment for all and as a trained doctor he focuses the debate on people accessing health care.
Community-led organizations have shown themselves to be an invaluable and essential part of our global public health infrastructure.
Strengthening them both financially and structurally has been demonstrated to enhance efforts to respond to HIV. The world will also be much better prepared to respond to the challenges that are coming—those we can anticipate and new health threats whose shapes we cannot yet envision.
The activism, mobilization and work of community-led organizations have defined the HIV response and saved countless lives.
Community-led organizations drive HIV responses in numerous ways. They demand that HIV programmes uphold people’s rights and dignity and highlight gaps and inequities. They advocate for legal and policy changes, and demand affordable access to medicines and services. They boost facility-centred programmes by making services more accessible, bringing community insights to planning and implementation, and by using grassroots monitoring to strengthen surveillance and accountability.
Studies show that community-led interventions can improve people’s HIV-related knowledge and attitudes, increase service access, and enhance prevention, treatment and care outcomes. They do that by providing services that are more convenient, relevant and efficient; by building trust and respect; and by reducing discriminatory practices. Those services can be more effective than standard health facility-based platforms in reaching marginalized and under-served populations, particularly when underpinned by capacity development.
Their adaptability of community-led services proved especially crucial during the first year of the COVID-19 pandemic, when community-led organizations set up medicine and food pick-up schemes and sites, arranged home deliveries, and shifted outreach work to virtual platforms.
Yet the value of community-led advocacy is still under-appreciated among many policy–makers and planners. This is reflected in the lack of financial and political support from governments in many countries. To perform their roles to the fullest, community organizations and networks need resources, including funding, training, and capacity building.
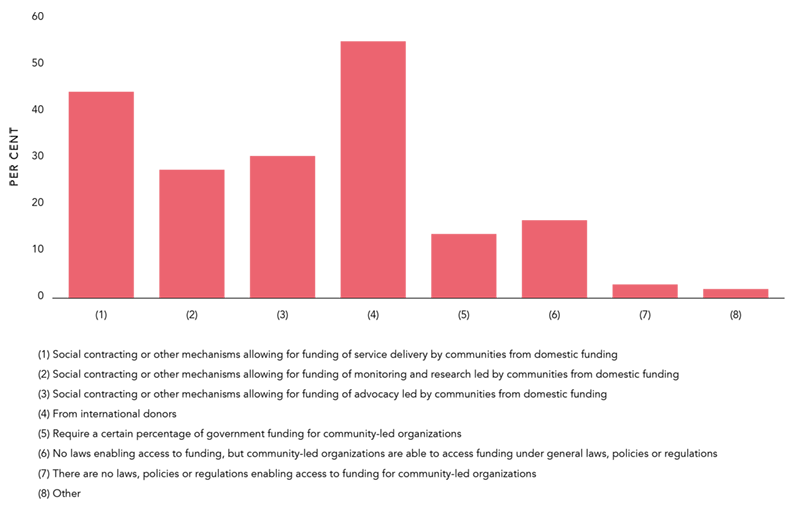
The activism, mobilization and on-the-ground work of community-led organizations have defined the HIV response and saved countless lives. In this chapter, read more about:
